
Powered By





Have you noticed itchy, flaky skin or unusual discoloration on your legs? This could be a sign of psoriasis, an autoimmune disease in which the immune system mistakenly targets the body’s skin cells. Although psoriasis symptoms can appear anywhere, they often show up on the knees, calves, shins, thighs, and even the toenails.
If your legs are itching and your dermatologist has diagnosed you with psoriasis, it’s important to understand how the condition works. Learning what causes symptoms and triggers flare-ups (periods when psoriasis gets worse) can help you find treatments to manage your symptoms so you feel more comfortable.
Symptoms of psoriasis on the legs are similar to those elsewhere on the body. The specific symptoms you experience will depend on your type of psoriasis. In general, psoriasis on the legs involves flaky patches that can become inflamed and scaly and often itch or burn.
Although most studies don’t focus on the location of psoriasis unless it’s out of the ordinary (like psoriasis on the feet or the hands), researchers estimate that 3 percent of people in the United States are living with some form of psoriasis. Because symptoms commonly develop on the knees, it makes sense that many people with this skin condition will have it on their legs at some point.

Here’s what you should know about the different types of psoriasis that can affect your legs.
Up to 80 percent of people with psoriasis have plaque psoriasis, making it the most common type. The raised patches are usually red or purple, depending on a person’s skin tone, and they often look scaly. On the legs, plaque psoriasis usually affects the knees, though it can show up anywhere.

About 25 percent of people with psoriasis develop inverse psoriasis. This type affects skin folds, where skin touches skin. Depending on your skin tone, you’ll see red, purple, or darkened patches that itch and burn but usually won’t get scaly. On your legs, you’re most likely to see inverse psoriasis at the top of the back of the thighs, under the fold of the buttocks, or possibly behind your knees.
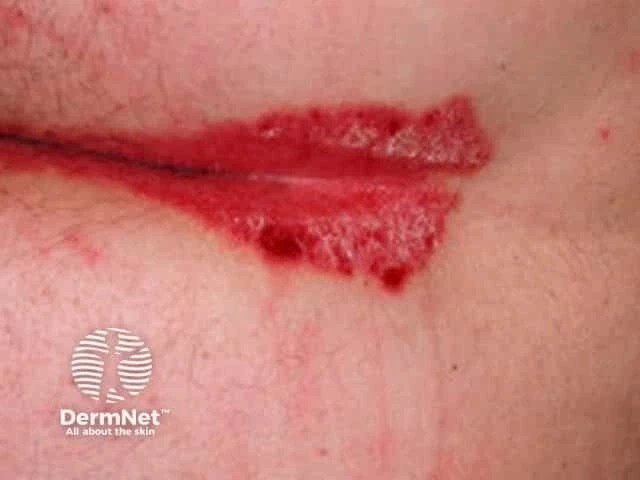
About 8 percent of people with psoriasis experience guttate psoriasis. It usually appears as papules — round, inflamed spots that may be red, purple, or just darker than the rest of your skin. These scaly papules commonly affect the legs but may also show up on other parts of the body.

Around 3 percent of people diagnosed with psoriasis have pustular psoriasis, which causes small, pus-filled bubbles or blisters. These pustules can appear anywhere on the body, so you may see pustular psoriasis on your legs.

Only 2 percent of people with psoriasis have a diagnosis of erythrodermic psoriasis. In this type, large areas of skin become red or purple, and all of that skin may shed at once. You may also get dehydrated, have severe pain or itching, and experience changes to your body temperature and heart rate. Erythrodermic psoriasis can affect all or most of your body, including your legs.

One MyPsoriasisTeam member described their condition this way: “The backs of my calves are scratched to death. Then comes the burn, and they feel like they are on fire.”
For many people, leg psoriasis isn’t just uncomfortable — it can interfere with everyday life, including sleep. “This psoriasis is all over me. Both knees and the top of my thighs hurt. I don’t sleep at night,” one member said.
When your legs itch or burn, it can be hard to find a comfortable position. Some people with psoriasis on their thighs or calves have trouble sitting, standing, or lying down for long periods. “I have a bad bout of it on the back of my thighs. It hurts to sit, and I can’t stand for long periods,” one MyPsoriasisTeam member shared.

Psoriasis symptoms on the legs can affect the way you feel about your appearance. A MyPsoriasisTeam member said their condition affects how they dress: “I have it badly on my calves, so I always wear a long dress or pants.”
Choosing clothing that feels good on your skin and helps you feel confident can make a difference. Soft, breathable fabrics, like cotton and bamboo, may help reduce irritation and make flare-ups feel more manageable.
Researchers don’t know exactly what causes psoriasis, but they believe an overactive immune system leads to skin changes. For instance, plaque psoriasis causes skin cells to multiply too quickly and build up, resulting in plaques, scales, and flakes. Researchers can’t yet predict where psoriasis symptoms will appear, so it’s not clear why it affects the legs for some people.

You’re more likely to get psoriasis if you have a family history of the condition. Other risk factors include smoking, having obesity, and taking certain medications, such as beta-blockers, lithium, or antimalarials. People who are living with human immunodeficiency virus (HIV) or recently had a streptococcal infection (like strep throat) also have a higher risk of psoriasis.
How do you treat psoriasis on the lower legs? Many treatment options are available. Your dermatology team can help you create a care plan based on your type of psoriasis and its severity, other health conditions, body type, lifestyle, and needs. They should fully explain how each treatment works, especially the way it’s given and any possible side effects.
For mild leg psoriasis, your healthcare provider will likely recommend starting with topical treatments such as gels, ointments, lotions, moisturizers, and creams. Topical treatments for psoriasis help hydrate your skin and may contain ingredients like:
Phosphodiesterase-4 (PDE4) inhibitors and aryl hydrocarbon receptor agonists also come in topical forms. Talk with your dermatology provider about your topical treatment options — some require a prescription.
Phototherapy, also called light therapy, involves exposing affected areas to certain types of light, usually several times a week for a month or more. There are several types of phototherapy, and your medical team will help you choose what’s best for you.
Because psoriasis is an autoimmune condition, treatment of severe cases often addresses the immune system directly. Your healthcare provider might recommend a medication like methotrexate or cyclosporine. In some cases, biologics may be prescribed. Newer systemic drugs, including Janus kinase (JAK) inhibitors and PDE4 inhibitors, are taken as oral pills.
Systemic treatment is usually prescribed for moderate to severe psoriasis when other therapies haven’t worked well enough. Your healthcare provider can help you understand potential side effects and balance the potential risks and benefits of this type of treatment.
If your psoriasis seems to flare up suddenly, a trigger might be to blame. Identifying and avoiding triggers won’t cure psoriasis but may help reduce flares and manage symptoms. Common triggers include:
If you have new or worsening psoriasis on your legs, or if your symptoms aren’t improving with treatment, talk with your healthcare provider right away. They can help you come up with a new treatment plan to help with healing and getting psoriasis flare-ups under control.
On MyPsoriasisTeam, people share their experiences with psoriasis, get advice, and find support from others who understand.
Are you living with psoriasis on your legs? What does it feel like? Let others know in the comments below.
Get updates directly to your inbox.



Hi, Can You Post Some More Information On Inverse Psoriasis. I Have Been Blessed With It And Would Like To Learn More About It. Thank You
Become a member to get even more




This is a member-feature!
Sign up for free to view article comments.
Are there natural treatments for staphylococcus aureus to remove it
We'd love to hear from you! Please share your name and email to post and read comments.
You'll also get the latest articles directly to your inbox.