
Powered By





Inverse psoriasis, also known as flexural or intertriginous psoriasis, is a rare and painful form of the inflammatory skin disease. It typically appears as smooth, shiny red patches in the armpits, genital and anal areas, and under the breasts. Symptoms of inverse psoriasis can worsen with warmth, moisture, and friction.
Between 3 percent and 7 percent of people with psoriasis have inverse psoriasis. It mainly affects infants and young children, but can appear at any age. Being overweight is believed to be a risk factor for inverse psoriasis. Among adults, inverse psoriasis most frequently occurs in the genital area. Up to 79 percent of people with this skin disease have lesions in the groin.
Because symptoms of inverse psoriasis can mimic other skin diseases, such as dermatitis, fungal or bacterial infections, or sexually transmitted diseases, it’s often difficult to diagnose. It’s also difficult to treat because of skin sensitivity in the affected areas. For this reason, it’s important to get an accurate diagnosis and proper treatment from a licensed dermatologist.
Like other types of psoriasis, inverse psoriasis is typically caused by an overactive immune system that creates inflammation and overproduction of skin cells, according to the American Academy of Dermatology (AAD). Scientists believe the disorder, a variant of plaque psoriasis — the most common form — may be caused by genetics or environmental factors. Stress, skin injuries, certain medications, and infections are all considered possible triggers. Allergies, diet, and even weather may also cause inverse psoriasis flares.
People with plaque psoriasis who are 20 or more pounds overweight may be at greater risk for also having inverse psoriasis, according to the AAD. Fatty tissue produces more cytokines — a type of protein that promotes inflammation — and can also lead to the development of psoriatic arthritis. Up to 45 percent of people who develop psoriatic arthritis are obese.
Inverse psoriasis generally covers a smaller body area than plaque psoriasis. Moisture, heat, and friction can aggravate symptoms.
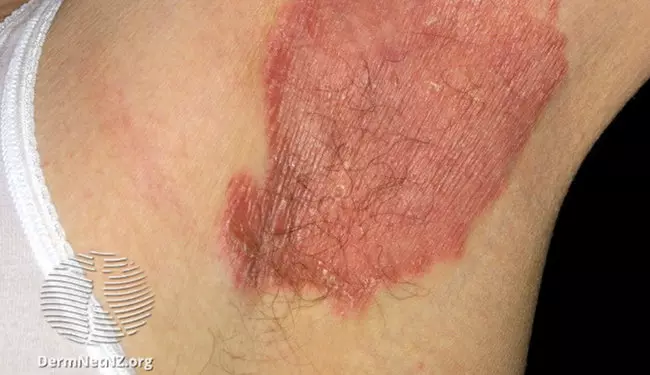
Common symptoms include:
Complications include the development of leathery, eczema-like irritations (lichenification) from rubbing or scratching the anal area. People with inverse psoriasis are also more prone to infections from medications that thin the skin. Sudden onset of inverse psoriasis may also signal HIV infection, some researchers suggest.
Lesions that occur in delicate skin folds distinguish inverse psoriasis from other types of psoriatic disease. Smooth red patches from skin-on-skin friction — particularly in the groin — can be a sign of inverse psoriasis. A dermatologist will perform a physical exam and visual inspection, and possibly take skin samples to confirm psoriasis and rule out any bacterial or fungal infection.
Treating inverse psoriasis can be challenging. Medications typically prescribed for plaque psoriasis and other types of psoriasis may irritate delicate skin affected by inverse psoriasis. Some topical preparations, such as Tazorac (tazarotene), can worsen symptoms in the genital area. Light therapy — including UVB, UVA, and laser treatments — and coal tar therapy can increase risk of genital cancer.
Treatment options for inverse psoriasis include topical medications and biologic drugs.
Topical corticosteroids — such as 1 percent to 2 percent hydrocortisone — are typically first-line therapies for inverse psoriasis, according to the National Psoriasis Foundation (NPF). Steroids temporarily control inflammatory response, reducing redness and swelling. Up to 85 percent of people report a reduction in itchiness and degree of lesions from topical steroids.
Low-strength steroids are typically recommended for the groin and breast areas in adults, but they should only be used for less than four weeks to avoid side effects. They’re safe for children as well, if used for short periods and applied only to small spots on the body. Steroids may also be combined with topical antiyeast or antifungal medications.
The nonsteroidal topical Dovonex (calcipotriene), a vitamin D compound, is sometimes recommended as a second or third-line treatment for inverse psoriasis. It doesn’t cause skin thinning, but it can be irritating. Topical calcineurin inhibitors for eczema — Protopic (tacrolimus) and Elidel (pimecrolimus) — may also be prescribed off-label for inverse psoriasis. They prevent the immune system from producing proteins that cause inflammation.
Biologic drugs — such as Humira (adalimumab), Stelara (ustekinumab), Remicade (infliximab), and Taltz (ixekizumab) — are sometimes prescribed to treat moderate or severe psoriasis that has not responded to topical treatment. Administered by injection or infusion, biologics change the way the immune system works by blocking the production of inflammation-promoting proteins. Some studies have found biologics to be particularly effective in clearing lesions from the rectal and genital area. Side effects include risk of infections.
Because itching, weeping, and other wound symptoms can worsen skin conditions, dermatologists recommend a regular practice of home care that protects skin against further irritation and injury. Simple changes like buying quality toilet paper, wearing loose-fitting underwear, and moisturizing can ease symptoms.
Skin affected by inverse psoriasis is prone to bacteria and odors. Frequent bathing in warm water using mild, chemical-free cleansers helps manage microbial build-up. Adding emollients such as bath oil or oatmeal to the water can soothe raw, painful skin. If odor continues, your doctor may order a bacterial culture.
Dermatologists recommend moisturizing after bathing, as well as periodically when skin areas feel dry. Eucerin, plain Aquaphor Healing Ointment, and other over-the-counter emollients help reduce chafing and irritation. They can be alternately applied with topical steroids and other medications.
Light, breathable underwear and clothing — loose-fitting boxers instead of briefs, for example — prevents skin irritation and discomfort. Cotton and other soft, natural fibers help prevent moisture from accumulating in the skin folds. Wash clothing in fragrance-free detergent and double rinse to ensure all soap has been removed.
Soft, high-quality toilet paper helps reduce irritation. Wiping the groin area gently but completely keeps genital lesions free of the bacteria in urine and feces that causes flare-ups.
Itching, one of the most problematic symptoms of inverse psoriasis, is important to carefully manage. That’s because scratching can create skin injuries that trigger flares and become infected. Using over-the-counter anti-itch and cooling lotions — as well as nonsedating antihistamine drugs by day and hydroxyzine at night — can help reduce the need to scratch. Aloe vera and jojoba oil can also soothe itching.
Chemical-free baby powder or cornstarch is often recommended to absorb moisture from weepy psoriasis lesions. Existing moisture should first be soaked up with a tissue before applying powder to prevent caking and build-up. Castederm (Castellani’s paint) is an over-the-counter liquid that’s painted onto skin to dry up moist skin fold lesions.
Dermatologists recommend cleansing skin in genital areas before and after intimacy to avoid rubbing medication onto your partner. Reapply medication after intercourse. Men are also advised to use lubricated condoms if either they or their partner has psoriasis, to reduce friction or injury. If your skin is raw in the genital area, postpone sex.
There is no known cure for inverse psoriasis, and the disorder has not been widely studied. However, inverse psoriasis is treatable and manageable. Talk with your doctor about treatments and lifestyle changes that can help you to be more comfortable.
Get updates directly to your inbox.



Can Inverse Psoriasis Come And Go In The Armpit Area?
Become a member to get even more




This is a member-feature!
Sign up for free to view article comments.
My 9 year old son has inverse psoriasis and we control it by eating a fairly strict but doable and delicious diet. We do the specific carbohydrate diet and allow a cheat here and there and it went… read more
We'd love to hear from you! Please share your name and email to post and read comments.
You'll also get the latest articles directly to your inbox.