
Powered By





Pustular psoriasis causes painful red skin with white, pus-filled bumps called pustules. Pustular psoriasis is not infectious or contagious. The pustules are considered sterile (germ-free) because they occur without an infection. Instead, overactivity of the immune system as a response to injury increases the white blood cells in the skin, causing the sores.
Pustular psoriasis is a rare form of the disease that is found in 3 percent of people with psoriasis. Generally, symptoms begin in infancy or first appear in middle-aged adults. Pustular psoriasis is more common in Asian populations.
Pustular psoriasis is a subtype of psoriasis. It causes lesions (cuts or sores) on specific patches of the skin. Pustular psoriasis may be further divided based on the location of these sores.
Palmoplantar pustulosis (PPP) causes sores on the palms of the hands and the soles of the feet. Smoking is known to increase a person’s risk for developing PPP.
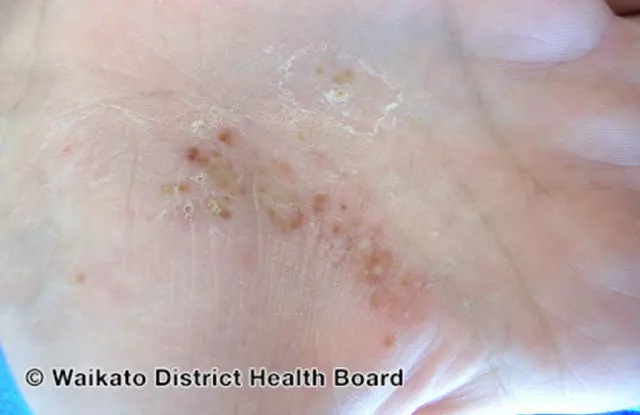
Pustular psoriasis (DermNet NZ)
Acrodermatitis continua of Hallopeau (also called acropustulosis) primarily involves the fingers and toes. It appears as yellowish-brown sores and skin discoloration.
Generalized pustular psoriasis (GPP) is a type of psoriasis that affects large areas of the body. GPP can also affect other organ systems such as the liver and kidneys. There are several subtypes of GPP.
A variation called von Zumbusch psoriasis causes diffuse sores over the body. It may also cause systemic (whole-body) symptoms such as fever, nausea, fatigue, and joint pain. This subtype is potentially life-threatening. Some people may have to go to the hospital if symptoms become severe.
Exanthematic psoriasis also involves diffuse sores. However, people with this subtype do not experience systemic symptoms. Lesions typically disappear within days.
Impetigo herpetiformis, also known as pustular psoriasis of pregnancy, is a form of GPP that occurs during pregnancy. It usually starts in the third trimester and may cause systemic symptoms.
Annular subtype psoriasis can be recognized by ring-shaped red patches with sores along the edge of the lesions. This subtype is more common in children than adults.

Watch dermatologist Dr. Raja Sivamani talk about pustular psoriasis.

Psoriasis is caused by the immune system responding when it should not. The exact causes of pustular psoriasis are still mostly unknown. However, some scientific studies have identified several genes that may contribute.
Some factors are also believed to trigger pustular psoriasis in people who have a genetic marker. Infections, ultraviolet light exposure, phototherapy, stress, pregnancy, and the use or discontinuation of certain medicines (such as steroids) may cause flare-ups.
Other medical conditions that increase inflammation can also contribute to the development of psoriasis, including pustular psoriasis. These can include conditions such as obesity, high blood pressure, high lipid levels, and diabetes, which all make pustular psoriasis more likely to occur.
Anyone with skin conditions such as scaly skin, eczema, blisters, or painful red skin should talk to a health care provider. If pustular psoriasis is suspected, a careful and thorough evaluation is important. Details about flare-ups and symptoms may help your doctor diagnose the specific type of psoriasis you are experiencing. Blood tests can be performed to detect increased inflammatory cells. Lesions can be swabbed to rule out infection and help with diagnosis.
In 2012, the American Academy of Dermatology developed treatment guidelines for pustular psoriasis. The goal of treatment is to reduce the frequency and duration of flare-ups and prevent complications. Pustular psoriasis can be difficult to treat. It may take time to develop an effective treatment that works for you, so discuss all treatment options with your dermatologist.
Oral retinoids are medications that are used to treat pustular psoriasis. The drugs work by reducing inflammation, swelling, and the growth of skin cells. Oral retinoids do not suppress the immune system, which helps to prevent infection. However, oral retinoids cannot be taken by anyone who is pregnant or may become pregnant.
Topical corticosteroids may be prescribed for flare-ups of pustular psoriasis. These steroids come in creams that are applied directly to the sores. They work by controlling inflammation. Steroids should not be used for extended time periods. It is important to follow instructions from your health care provider. Sudden discontinued use can worsen or trigger flare-ups.
Biologics are approved for the treatment of psoriasis. These medications target and block inflammatory signals in the body. Biologics are considered first- or second-line therapy for people with pustular psoriasis and include:
Coal tar is one of the oldest treatments for psoriasis. It is used to this day because it is very effective. It can also be used long term. Coal tar can be found as an over-the-counter treatment in the form of bathing solutions, ointments, and lotions. It is a good treatment option for pustular psoriasis and sores on the palms of the hands and soles of the feet.
Vitamin D helps regulate the skin and the immune system. Vitamin D may be helpful for some people, but it should be used with the guidance of a health care provider to avoid side effects.
Phototherapy uses a specific type of UV light on skin lesions to reduce skin growth. It also suppresses the immune system. Research has shown that phototherapy can be effective for treating palmoplantar psoriasis. Phototherapy should be avoided in people who have had skin cancer or are sensitive to UV light.
Cyclosporine and methotrexate are drugs that reduce the responsiveness of the immune system. They are used to treat severe psoriasis that has not responded to other treatment options. By reducing the activity of the immune system, they quickly manage psoriasis symptoms. However, they also have potentially serious side effects such as kidney damage and increased risk of infection. Otezla (apremilast) is another medication that can be used as a disease-modifying antirheumatic drug. It requires less monitoring than cyclosporine or methotrexate.
MyPsoriasisTeam is the social network for people with psoriasis and their loved ones. More than 89,000 members come together to ask questions, give advice, and share their stories with others who understand life with psoriasis.
Do you have symptoms of pustular psoriasis? Share your experience in the comments below, or start a conversation by posting on MyPsoriasisTeam.
Get updates directly to your inbox.



Any recommended remedies for the itching, stinging & burning pain with pustular psoriasis
Become a member to get even more




This is a member-feature!
Sign up for free to view article comments.
I have had pustular psoriasis for a long time and my flair ups vary from time to time to time. I notice mine start with my face (hairline) and back of neck and on my back between my shoulder blaids.
… read moreWe'd love to hear from you! Please share your name and email to post and read comments.
You'll also get the latest articles directly to your inbox.